

Cancer is personal. Time is a commodity, and the public health service does not always have the resources to save your life. Long queues, limited access to life saving treatments, and dismal outcomes are the everyday reality of cancer patients relying solely on the public health service. At GlobMed, we offer patients a better option; a patient centred approach to cancer treatment.
We have partnered with the regional leader in oncology treatment in Europe. Created in affiliation with Johns Hopkins Medicine in 2005, our oncology partner has an established track record of providing high quality cancer care, especially to international patients. Your highly trained oncologists and medical team will review your case with due diligence and respect to your treatment goals.
There is no perfect solution and no “one size fits all” when it comes to treating cancer. Through our world-leading partners, we can offer patients industry-leading technology in oncological treatments (PET-CT, CyberKnife, TrueBeam, Radixact). These leading programs are conducted by a team of internationally experienced doctors, trained in America, and well-recognized in Europe and abroad. Your medical team will have access to specialists from Johns Hopkins for providing medical second opinions and tele-conference briefings.
Certified by multiple international organisations, JCI (Joint Commission International), ESMO (European Society for Medical Oncology), and Planetree Gold Certification on Person Centred Care, you can expect to receive American-style quality healthcare.
Cancer is characterised by the uncontrolled and rapid multiplication of cells. Although some cell types, such as those in the skin and stomach, undergo frequent turnover, under normal circumstances, this process is tightly regulated.
When cancer develops, the body's usual control mechanisms fail to manage the accelerated replication and division of cells. Cancer can arise anywhere in the body and can affect any type of cell.
As part of a typically well-regulated and natural process, old or damaged cells die off, making room for new cells. However, when this process malfunctions, it can result in abnormal cell division and growth, leading to an uncontrollable replication of cells. These abnormal cells may cluster together to form masses of tissue known as tumours. Tumours can either be cancerous (malignant) or non-cancerous (benign).
It is, in many cases, impossible to identify and determine the precise cause of cancer. However, there are a number of risk factors and influencing factors that can play a part in developing cancer.
There are various potential risk factors when it comes to the causes of cancer and the factors which may increase the chances of getting cancer in the first place. Although some genetic factors and family genetic history can affect the chances of getting cancer (such as having a BRCA gene in the case of breast cancer), there are additional external factors to consider too.
Although some of these risk factors can be avoided, others, such as growing older, cannot. Reducing these external risk factors and improving one’s lifestyle where possible can contribute to a reduction in the chances of getting cancer - common external factors that can contribute to getting cancer include:

The risk of developing cancer can be influenced by various factors, including lifestyle choices, genetic predispositions, family history, and the broader environmental context in which we live.
Continuous advancements in cancer research are unveiling innovative methods to tackle and treat this disease. Among these are potential preventive measures that can be taken to lower the risk of cancer:
In 2019, around 391,000 people were diagnosed with cancer in the UK.
In England, over a third of the population is projected to be diagnosed with cancer during their lifetime. Furthermore, cancer accounts for one in every four deaths in the UK. This grim reality translates to over 200,000 new cancer diagnoses annually, with approximately 120,000 people succumbing to the disease each year in the UK alone.
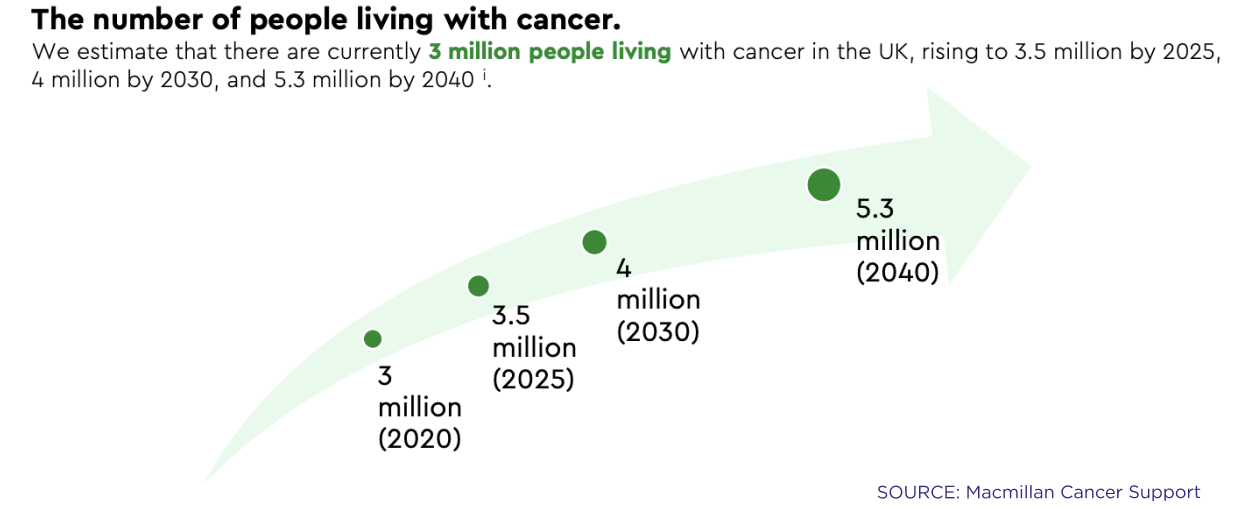
There are many different types and sub-types of cancer and the prevalance of the different types differ between regions and demographics.
Should you present symptoms or receive a screening test result indicative of cancer, your doctor is obligated to investigate whether this is indeed due to cancer or some other underlying condition. This investigation may commence with an assessment of your personal and familial medical history, coupled with a physical examination. Your doctor might also request laboratory tests, imaging scans, or other diagnostic procedures. A biopsy may be necessary, as it often serves as the most definitive means of confirming a cancer diagnosis.
Biopsies involve the extraction of tissue samples from the body for examination under a microscope. In cancer diagnosis, biopsies are crucial for confirming the presence of cancer..., determining its type, and assessing its characteristics. This procedure helps oncologists make accurate diagnoses and develop appropriate treatment plans for patients.
A CT scans utilise x-rays, linked to a computer to take a series of pictures of your organs from a variety of different angles. These pictures are used to create detailed 3-D images of the inside of your body.
An MRI scan uses powerful magnetic waves as well as radio waves to capture pictures of your body in portions or ‘slices.’ These portions are then collated and used to create much more detailed images of the inside of the patient’s body, which can differentiate between healthy and unhealthy tissue and in some cases, cancerous or non cancerous tissue.
Nuclear scans use radioactive material to capture images of the inside of you body. Before a patient can undergo this type of scan, a small amount of radioactive material is injected into their body, so that it flows through their bloodstream and collects in bones or organs, highlighting cancerous cells.
Bone scans are a type of nuclear scan that checks for abnormal areas, growths and damage in bones. They are typically used to diagnose bone cancers or cancers that have metastasised to the bones (also called metastatic bone tumours).
A PET scan is another form of nuclear scan that takes very detailed 3-D images of specific areas inside the body where glucose is absorbed. Cancer cells will often take up more glucose than normal healthy cells, allowing the scans to locate and identify cancer in the body.
Ultrasound scans use high-energy sound waves that people cannot hear. The sound waves echo off tissues inside your body. A computer will then use these echoes and the sound waves to generate an accurate image of an area in your body, known as a sonogram.
X-rays are a form of electromagnetic radiation that can pass through objects, including the human body. In cancer diagnosis, X-rays are commonly used to create images of internal structures, such as bones and organs, helping detect abnormalities like tumors.
Lab tests involve analysing samples of blood, urine, tissue, or other bodily fluids to detect abnormalities. In cancer diagnosis, these tests help identify tumor markers, genetic mutations, and other biomarkers that indicate the presence of cancer cells, aid in determining the type and stage of cancer, and guide treatment decisions.
The primary goal of cancer treatment is to cure the disease, to completely remove cancer from the patient's body. However, if a complete cure isn't achievable, the focus shifts to control, that is, to limit the growth or slow the progression of cancer, treating it as a chronic disease.
In instances where controlling the cancer growth is not possible, palliation becomes the priority. This involves improving the patient's quality of life by alleviating symptoms such as pain and breathlessness associated with the disease, a practice often termed as palliative or supportive care.
These specific objectives are contingent on various factors, including the type and stage of cancer, potential side effects, the patient's overall health, and personal preferences. Ongoing research continuously strives to develop novel therapies aimed at enhancing effectiveness, reducing side effects, and improving the quality of life during and after treatment.
Chemotherapy is a cancer treatment that uses drugs to stop cancer cells from growing and dividing. It can be employed individually or alongside other treatments like surgery or radiotherapy. Though effective, chemotherapy can affect healthy cells, causing side effects like fatigue and hair loss. Treatment specifics depend on the cancer type, its stage, the patient's health, and treatment goals.
Learn More
Immunotherapy is a type of cancer treatment that helps your immune system fight cancer. The immune system helps your body fight infections and other diseases. It is made up of white blood cells and organs and tissues of the lymph system. Several types of immunotherapy are used to treat cancer.
Learn More
Surgery is a common method of treating cancer in the UK, involving the removal of the tumour and surrounding tissue. It can be used alone or in combination with other treatments such as chemotherapy or radiotherapy. The aim is to remove all visible cancer, aiding in full recovery or prolonging life.
Learn More
Radiotherapy uses high-energy radiation to destroy cancer cells' DNA, inhibiting their growth and division. Radiotherapy can be used independently or alongside other treatments like surgery or chemotherapy to enhance the overall effectiveness of cancer management.
Learn More
Simply contact us and our Health+ Consultant will be in touch within 24 hours.
Contact Us